Lyme Disease: What to do after a deer tick bite – Procedure following removal of a deer tick – To treat or not to treat preventively – Best Testing Practices
Patient Instructions from Dr. Richard Maurer
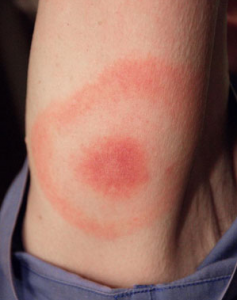
Bull’s Eye Rash – No blood test needed – diagnosis is clear: Lyme+
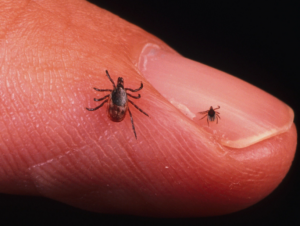
That teeny one is the nymph and yes – it can carry lyme too.
I live and practice in an area with prolific deer ticks and these ticks often carry bacteria, the most notorious of which is Borrelia species which causes Lyme disease. To transmit the bacteria from their belly to your bloodstream requires them to be on long enough to feed. While some resources say this takes 24-48 hours, the tick can clearly reach a blood meal environment sooner. So removal asap is key.
The tick should be removed by grabbing as close to the head as possible, don’t squeeze the belly. Pull straight out. The tick
will seem imbedded as soon as the “anchors” are set. This, does not mean it has been feeding, only that it has anchored. The tick typically takes 12-24 hours to start feeding, so there is time to remove the tick before exposure to harmful bacteria. Here is a nice description of how to remove the tick.
TO DOSE an Antibiotic (doxycycline) preventively or NOT? I do not.
There is a protocol that recommends using a single dose of 200-mg of doxycycline the day the tick is removed. A study showed that the single dose doxy reduced the rate of rash and acute symptoms compared with those who did not do the single dose. I have a concern with this practice! Subjects were not followed long-term (>3 months) and the single dose might have only slowed the bacteria down causing a more gradual and complex Lyme disease scenario down the line. Since I do not think think there is evidence that a single dose effectively kills the Borrelia bacteria or the possible co-infections (other bacteria that the ticks transmit to humans) – I’d rather assess whether the bacteria was truly transmitted and if so, treat aggressively with proper drug, dose and duration.
If the tick was there for greater than 24 hours, there are a few steps to take. Mark the date on the calendar, save the tick for proper ID if you are unsure, and circle the spot on your skin so you remember where it was. The first few days after removal, it is red due to the bite itself, not the bacteria. The “Bulls Eye Rash” shows up in perhaps 60% of the cases and shows up between 3 days and 3 weeks after the bite. So watch carefully. Any fever or joint pain during this time is highly suspect and may warrant immediate treatment.
When and how to run the most accurate test.
If there are no symptoms, run a western blot test about 3 weeks post-tick bite [3 weeks to 3 months is the best window to get a positive test if the infection is present]. DO NOT LET YOUR DOCTOR RUN THE SCREENING TEST ONLY. Go right to the Western blot – this checks IgG and IgM antibodies to the fragments of Borrelia bacteria. You can request this test directly, anywhere in the U.S. HERE at ULTA LAB TESTS, it’s only $63.00. But again, symptoms in this first 3-week period will guide treatment, blood tests are rarely positive prior to 3 weeks post bite. If you are on anti-histamines or steroids, you may not get the tell-tale rash, this makes diagnosis more difficult. If you are on steroids, the suppression of the immune response may also make diagnosis by symptoms more difficult AND the blood test may falsely test normal due to the suppression of your immune antibodies. In these cases, a test at 3 weeks post-tick bite is the best way to proceed. You need as certain a diagnosis as possible; treatment is typically high dose antibiotics for an extended period of time. I don’t recommend treatment flippantly. The antibiotic is harmful in and of itself…but a necessary cost for the benefit of effective eradication of Lyme bacteria. The relapse rate with 3-weeks of antibiotics is too high and I therefore recommend (and have used personally) antibiotics for greater than 4-weeks for effective treatment of Lyme disease. Again, I can’t emphasize enough that early and accurate diagnosis is paramount, so get in to see your doctor to assess any symptoms that arise in the weeks following a tick bite. The bacteria is pretty vulnerable early-on so it can be effectively treated with antibiotics and supportive therapies.
Co-infections can be a concern and there are different blood tests for these. Fortunately in my experience, they are more responsive to treatment and don’t require the long course of antibiotics. Find a provider to test for these infections if Lyme is testing negative and symptoms of infection (like fatigue, fever) persist. Don’t let these symptoms go unaddressed.
BTW: For those on antibiotics – I like to use Garlicin (1 tablet 2x/day away from the antibiotic) and Primadophilus original (2 capsules twice daily away from the antibiotic) adjectively. Furthermore, if you know you have lyme, you will need to request treatment be extended PAST the typical three-week mark. Six-weeks is my minimum in clinical practice.
Dr. Maurer



Comments are closed.